BRCA testing used to cost $3,000. Now you can screen for €99.
BRCA1 and BRCA2 mutations are responsible for most hereditary breast and ovarian cancers. We screen your DNA for pathogenic variants in 6 cancer-risk genes — BRCA1, BRCA2, MLH1, MSH2, TP53, and CHEK2 — using the same medical databases your doctor uses. Not a diagnosis. A screening that tells you if you should get clinical follow-up.
 ClinVarNIHNCCN GuidelinesNational Cancer Institute
ClinVarNIHNCCN GuidelinesNational Cancer InstituteWhat are BRCA genes?
BRCA1 and BRCA2 are tumor suppressor genes. When they work correctly, they repair damaged DNA and prevent cells from growing out of control. When they carry a pathogenic mutation, this repair mechanism breaks down — significantly increasing cancer risk. About 1 in 400 people carry a BRCA mutation. If you have a family history, the odds may be higher.
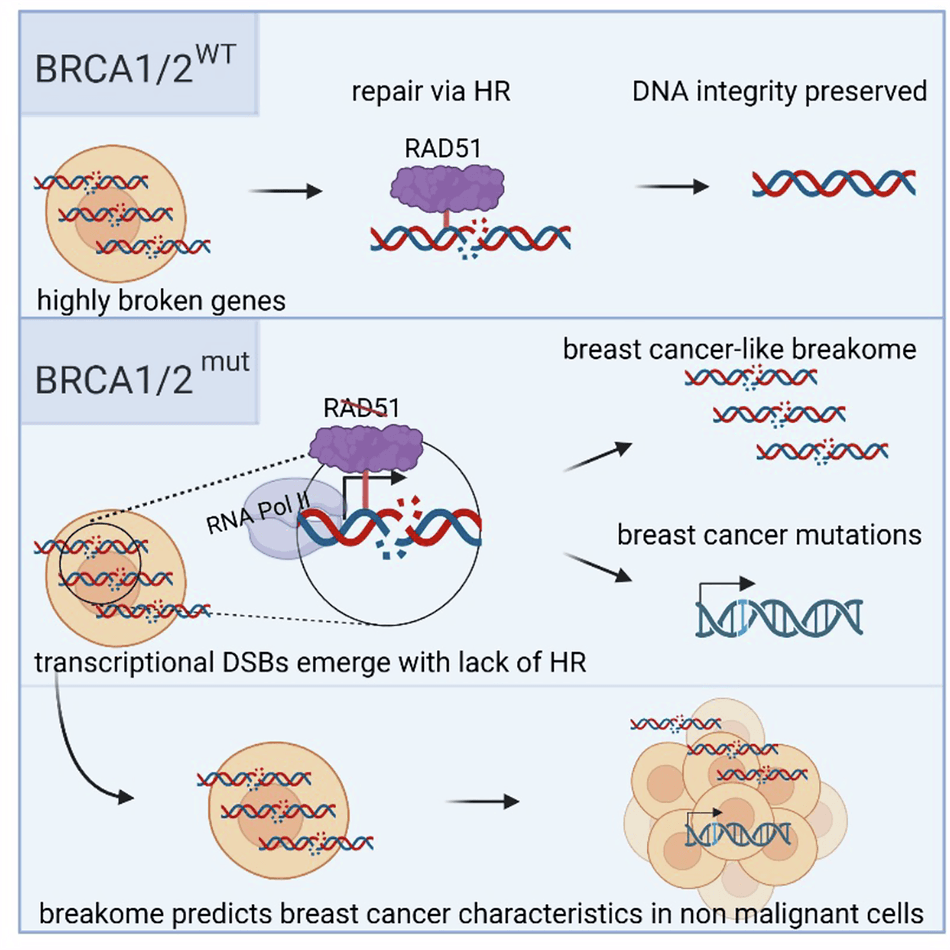
DNA repair genes
BRCA1 and BRCA2 are part of your body's DNA repair system. A pathogenic mutation means your cells can't fix DNA damage as well, increasing cancer risk over time.
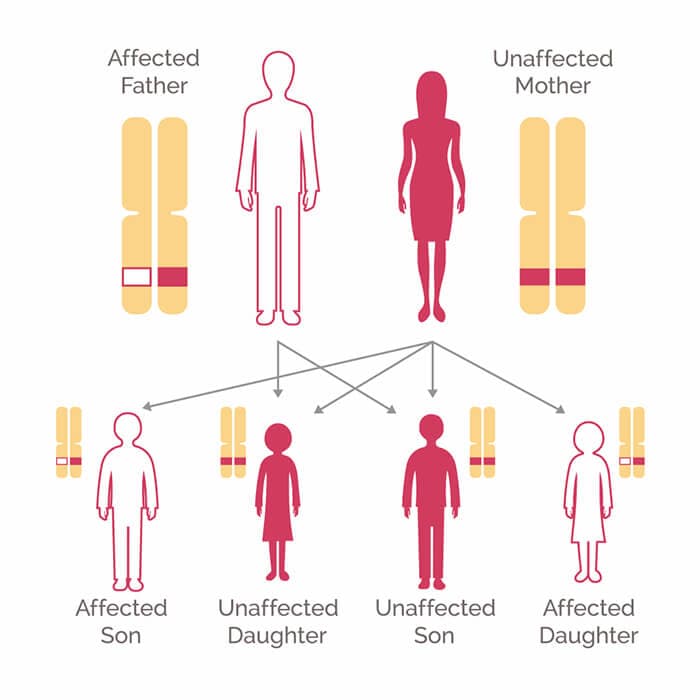
Hereditary — passed through families
BRCA mutations are inherited. If a parent carries one, each child has a 50% chance of inheriting it. Family history of breast, ovarian, or pancreatic cancer is a key indicator.
Affects both women and men
Women face breast and ovarian cancer risk. Men with BRCA2 have increased breast and prostate cancer risk. Lynch syndrome genes affect colorectal cancer risk for everyone.
Early awareness saves lives
People who know their BRCA status get screened earlier, catch cancers at earlier stages, and have significantly better outcomes. Knowledge turns risk into a plan.
Screen your DNA for hereditary cancer risk genes.
Upload your 23andMe or AncestryDNA file. Results in 2 minutes.
The numbers, in context
Carrying a BRCA mutation does not mean you will get cancer. It means your risk is higher than average — and knowing that risk gives you the power to act.
General population
Lifetime breast cancer risk
Lifetime ovarian cancer risk
BRCA1 carrier
Lifetime breast cancer risk
Lifetime ovarian cancer risk
BRCA2 carrier
Lifetime breast cancer risk
Lifetime ovarian cancer risk
Important:These risk figures come from large population studies (NCCN, National Cancer Institute). Your individual risk depends on mutation type, family history, lifestyle, and other factors. A positive screening result is a reason to talk to a genetic counselor — not a reason to panic.
6 cancer-risk genes, one report
We go beyond BRCA. Our screening covers the most clinically actionable hereditary cancer genes recognized by NCCN guidelines.
BRCA1
Breast & ovarian cancer
Most studied hereditary cancer gene. Pathogenic variants dramatically increase lifetime risk.
BRCA2
Breast, ovarian & pancreatic cancer
Similar to BRCA1 with additional associations to pancreatic and prostate cancer in males.
MLH1 / MSH2
Lynch syndrome (colorectal, endometrial)
Lynch syndrome accounts for 3-5% of all colorectal cancers. Early screening saves lives.
TP53
Li-Fraumeni syndrome (multiple cancers)
Rare but highly penetrant. Associated with breast, brain, adrenal, and soft tissue cancers.
CHEK2
Breast cancer (moderate risk)
Moderate-risk gene. Carriers may benefit from earlier or more frequent screening.
PALB2
Breast cancer
Works closely with BRCA2 in DNA repair. Recognized by NCCN as high-risk gene.
Risk figures from NCCN Guidelines, National Cancer Institute, and peer-reviewed studies.
Screening is the first step. Early awareness saves lives.
Same DNA file you already have from 23andMe or AncestryDNA.
What to do with your results
Whether your screening is clear or flags something, here's what to do next.
If no pathogenic variants found
- Good news — but remember: consumer DNA chips don't catch every mutation. A negative screening does not rule out all hereditary cancer risk.
- If you have strong family history, discuss full gene sequencing with a genetic counselor.
- Continue age-appropriate cancer screening (mammograms, colonoscopies) as recommended by your doctor.
If a pathogenic variant is flagged
- Don't panic. A screening result needs confirmation with clinical-grade genetic testing.
- Schedule an appointment with a genetic counselor. They can order confirmatory testing and discuss what your results mean for you and your family.
- If confirmed, your doctor will create a personalized surveillance plan: earlier mammograms, breast MRIs, CA-125 monitoring, or colonoscopies depending on the gene.
- Use our physician summary to give your doctor the variant details, ClinVar classification, and research references.
Three steps to your screening
Upload your DNA file
23andMe, AncestryDNA, Nebula, MyHeritage, or any VCF file. It takes 30 seconds.
We screen your cancer-risk genes
We check BRCA1, BRCA2, MLH1, MSH2, TP53, CHEK2, and PALB2 against ClinVar, NCCN guidelines, and 13 more medical sources.
Get your screening report
Variant status, ClinVar classification, risk context, next steps, and a physician-ready summary to bring to your doctor.
Early awareness changes outcomes

Caught my cancer because of Promethease... brought in my report to push for a biopsy.
— Reddit user (+156 upvotes)
My mother and grandmother both had breast cancer. I needed to know if I carry the gene. Turns out I do. Got my first MRI at 30 instead of waiting until 40.
— Reddit user
Promethease indicated I have a pathogenic BRCA1 variant. Medical-grade testing confirmed it. That $15 test may have saved my life.
— Reddit user
1 in 400
people carry a BRCA mutation
6
cancer-risk genes screened
2.6M
genetic markers cross-checked
15
medical sources
Common questions
Screening,
not diagnosis.
Early awareness is the single most powerful tool against hereditary cancer. Your DNA file already contains the answers — you just need the right analysis.